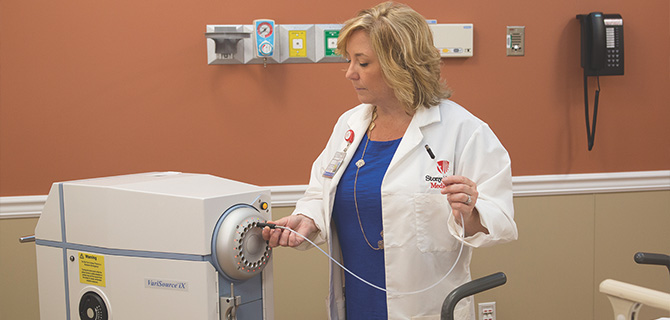
Brachytherapy is a radiation treatment method by placing radioisotopes within or on the tumor. At Stony Brook, we have a long experience with brachytherapy, and we use the most advanced brachytherapy treatment system.
The VariSource iX® system is a completely automated high-dose-rate (HDR) after-loading system. Physicians are able to use catheters to place small radioisotope seeds (such as Iridium-192) directly within the tumor, or in body cavities or tissues, often under anesthesia or sedation. Depending on the size and shape of the tumor, multiple catheters can be used. Using the VariSource iX, the radioisotope source travels through the catheter(s) to the target within the tumor or body cavities. Once the dose is delivered, the sources are safely retracted back to the container, making this process extremely precise and safe. At Stony Brook, this treatment modality is performed using an advanced image-guidance system and takes place in the new highly equipped brachytherapy HDR suite. Brachytherapy is used to treat prostate cancer, skin cancer, gynecological cancer, esophageal cancer, and tracheobronchial cancers.
HDR Gynecological Treatment
Vaginal Cylinder treatments are most commonly performed on patients who have had a hysterectomy. In this scenario the applicator has a central metallic tube in which the radioactive source will travel. The cylinder is inserted into the vagina and will remain there for the duration of the treatment. Typically, the total preparation and treatment time for the first day is a couple of hours while the remaining days are about an hour.
HDR Brachytherapy for cervical or endometrial (uterine) cancers is typically done using a "tandem and ovoid" (T&O) applicator, which reaches both the cervix and uterus. The tandem is a long, thin metal tube that is passed through the cervix, into the uterus. The ovoids are circular hollow capsules placed in the vagina, pressed against the cervix. Once placed in the vagina, the applicator is connected to a machine that automatically feeds a radiation source into the applicator, where it remains for a predetermined time, known as the dwell time. Once the time is up, the machine removes the source and the applicator is removed from your vagina. The dwell time can be anywhere from 15-25 minutes.
HDR Skin Treatment
HDR brachytherapy is an effective treatment option for patients with localized non-melanoma skin cancer (NMSC), specifically when the tumor cannot be removed surgically because of location or shape, without a poor cosmetic result. The use of HDR brachytherapy for the treatment of NMSCs is typically limited to superficial tumors (depth ≤5 mm).
To perform HDR Skin Treatment, the catheters are incorporated in a surface mold in a non-invasive manner. In our practice, a technician creates a thermoplastic mesh of the patient’s body surface in the region of interest. The thermoplastic mesh helps to restrict the patient’s movement during treatment. Catheters are fixed in the mold using wax pieces. The catheter placements are evenly distributed over the region of interest so that the radioactive sources can deliver radiation to all cancerous tissue. The purpose of the wax surface mold is to restrict the movement of the catheters during the entirety of the treatment process.
HDR Prostate Cancer Implant Therapy
In the past, prostate permanent implant therapy was widely used. However, the patient carries radioactivity within their body for a while. We offer HDR temporary implant within the prostate in one or two sessions, each one 3-4 hours under sedation or anesthesia. The patients do not have any radioactivity and return to normal daily activity immediately after the treatment.